Aug 25, 2017 | Healthy Tips

TIRED OF YOUR DIABETES? HERE’S HOW TO KEEP GOING
By David Steen Martin
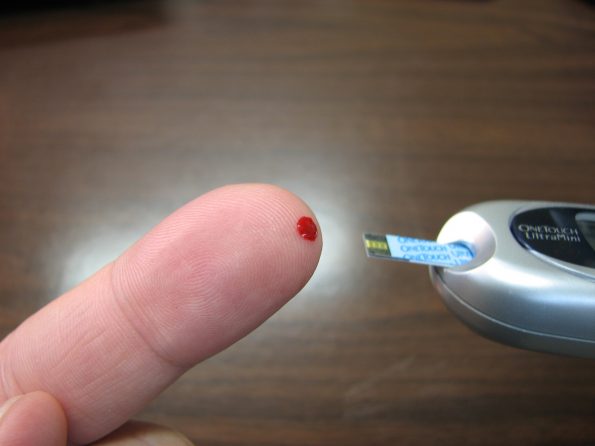
When you have diabetes, your daily to-do list can seem like a lot. You track your blood sugar, take medicine, watch your diet, and exercise.
It can make you feel overwhelmed and burned out. If you’re there:
- Know that no one is perfect.
There are no vacations from diabetes. Even the most diligent people can’t keep their blood sugar or diet or physical activity on target all the time.
“Diabetes is unique because [you’re] actually making medical decisions, day-to-day, minute-to-minute,” says Alicia McAuliffe-Fogarty, Ph.D., a clinical health psychologist.
This can be stressful, says David Nathan, MD, director of the Diabetes Center at Massachusetts General Hospital.
“If people are always stressed out about diabetes, they’re miserable,” Nathan says.
He says people need to forgive themselves if they miss their goals for a day, a week, or even more.
“Chill a little bit,” Nathan says. “We’re going to do the best we can. We need to recognize no one is perfect.”
- Pay attention to what stresses you out.
Living with diabetes can cause fear, anger, worry, and sadness.
Lawrence Fisher, Ph.D., director of the Behavioural Diabetes Research Group at UCSF School of Medicine, has studied what doctors call “diabetes distress” in people with type 1 and those with type 2 diabetes. He learned that during any 18-month period, from a third to a half of people with diabetes will feel a good bit of it.
He cites seven common sources of diabetes distress among people with type 1 diabetes. The most common is a feeling of helplessness.
“The [blood sugar] numbers have a life of their own. They go up. They go down. You’re constantly making adjustments,” Fisher says. “There’s a feeling of powerlessness that is really hard to tolerate.”
Other common sources of diabetes distress among people with type 1 diabetes include:
- Worry about what those around them assume
- Concern about access to good health care
- Perceived lack of support from family or friends, or feeling like they’re the “diabetes police”
- Fear of dangerously low blood sugar
- Stress over managing blood sugar levels
- Bother over what to eat and when
- Fisher says people with diabetes should pay attention to what stresses them out and try to address those things. He suggests programs or workshops that focus on what gets you down.
- “There are things you can do,” he says.
- He found that people with type 2 diabetes also had a feeling of helplessness. A sense of failure and negative social perceptions were other common sources of bother among type 2 folks, he says.
- Paying attention to what gets to you about your diabetes is important. The less spun-out you are, the better you’ll be able to manage your disease.
- Set realistic goals.
- That’s important to avoid burnout. It can mean taking a big goal and breaking it into more manageable pieces.
- “Taking small steps to achieve a larger goal often makes sense,” says McAuliffe-Fogarty, who has type 1 diabetes.
- If you need to lose 50 pounds, shoot for 2 pounds a month, she says. If you drink regular soda, try switching to diet. If you normally eat a pint of ice cream, switch to a half a pint.
- “You should adapt your treatment plan to your lifestyle rather than the other way around,” says McAuliffe-Fogarty, who is also vice president of the lifestyle management team at the American Diabetes Association.
- Ask for help.
- Build a support network — and use it.
- In addition to your doctors, look for counsellors or family friends who can be there for you when you feel down. Sharing stories as part of a diabetes support group can be very helpful.
- Ask those closest to you for specific help you need. This can be anything from asking a family member to remind you to take your medication to asking a friend to go for a walk with you a few times a week, McAuliffe-Fogarty says.
- “Without that support, people often get down,” she says.
- Know transitions can be hard.
- Change can be a challenge for anyone. Going through it while you manage your diabetes can be really tough.
- Heading to college, being diagnosed with a complication, and trying a new treatment are types of adjustments that can bring worry, McAuliffe-Fogarty says.
- To ease stress, try to anticipate and prepare for big changes in your life. That’ll lessen the impact on how you manage your diabetes.
- Tell your doctor all about it.
- See him regularly. When you go, make sure to share your physical symptoms, and how you’re feeling about things. Your diabetes can make it more likely for you to be depressed or anxious. What’s more, how you feel plays a big role in your ability to control your diabetes.
- “That’s a component that’s often forgotten or left out,” McAuliffe-Fogarty says of mental well-being. “It’s equally important as eating right and exercising.”
- It’s important that you take an active role in communicating with your doctor. He’s trained in managing diabetes. But he may not be as knowledgeable about the emotional toll the disease can take, McAuliffe-Fogarty says.
Aug 25, 2017 | Healthy Tips

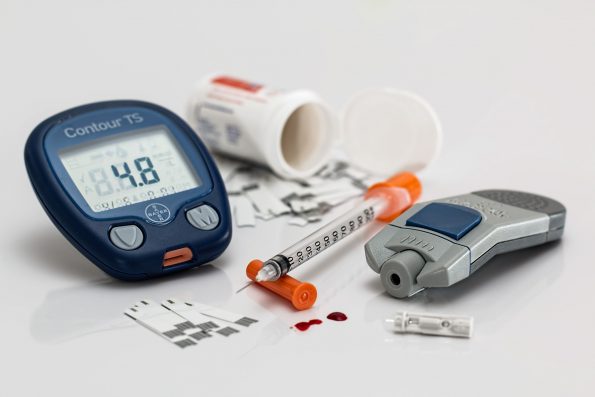
HOW TO LOWER YOUR RISK- DIABETES
Good habits go a long way toward preventing the other health problems that diabetes can cause. Make these tips part of your regular health routine:
Keep tight control of your blood sugar. It’s the best way to avoid diabetes complications. Your levels should stay in these healthy ranges as much as possible:
• Between 70 and 130 mg/dL before meals
• Less than 180 mg/dL 2 hours after you start a meal
• Glycated hemoglobin or A1C level around 7%
Watch your blood pressure and cholesterol. If they’re too high, you’re more likely to get other health problems, like heart disease. Try to keep your BP below 140/90, and your total cholesterol at or below 200 mg/dL.
Get regular check-ups. Your doctor can check your blood, urine, and do other tests to spot any problems. These visits are especially important since many diabetes complications don’t have clear warning signs.
Don’t smoke. Lighting up harms your blood flow and raises blood pressure. If you need help to quit, your doctor can recommend treatments that might work for you.
Protect your eyes. Get a yearly eye exam. Your doctor can look for damage or diseases.
Check your feet every day. Look for any cuts, sores, scrapes, blisters, ingrown toenails, redness, or swelling. Wash and dry your feet carefully each day. Use lotion to avoid dry skin or cracked heels. Wear shoes on hot pavement or on the beach, and socks and shoes in cold weather. Test bath water before you get into avoid burns on your feet. Keep your toenails trimmed and filed straight across.
Take care of your skin. Keep it clean and dry. Use talcum powder in places where skin may rub together, like your armpits. Don’t take very hot showers or baths, or use drying soaps or bath gels. Moisturize your skin with body and hand lotion. Stay warm in cold winter months. Use a humidifier in your bedroom if it feels too dry.
WebMD Medical Reference
Reviewed by Minesh Khatri, MD
Aug 25, 2017 | Healthy Tips

METH ABUSE COULD UP STROKE RISK IN YOUNGER USERS
THURSDAY, Aug. 24, 2017 (HealthDay News) —
Younger adults who use methamphetamine may be at greater risk for stroke, a new review suggests. With the use of the stimulant increasing, particularly in more potent forms, doctors in many countries are seeing more meth-related disease and harms, the Australian study authors said. This is especially true among younger people, who are the major users of the drug.
“It is likely that methamphetamine abuse is making a disproportionate contribution to the increased incidence of stroke among young people observed over recent years,” said researchers led by Julia Lappin. She’s with the National Drug and Alcohol Research Centre at the University of New South Wales in Sydney.
These strokes can lead to disabilities or death, she and her colleagues pointed out.
For the review, Lappin’s team analyzed 77 studies that investigated the link between methamphetamine use and stroke risk in adults younger than 45. They identified reports of 98 strokes — 81 caused by bleeding into the brain (hemorrhagic) and 17 caused by a blood clot (ischemic). Men were twice as likely as women to suffer one of these strokes.
Ischemic strokes are more common in the general population.
But eight out of 10 of the strokes associated with methamphetamine abuse were bleeding strokes, the researchers said. This is a dramatically higher rate than typically reported among people in this age group and older adults.
The brain bleeds also increased the risk of death among younger methamphetamine users: One-third of them died, the study found.
Bleeding strokes were associated with the drug regardless of whether it was swallowed or injected. In about one-third of all cases, the strokes were linked to inflamed blood vessels and high blood pressure, the researchers said.
They added that methamphetamine abuse could cause high blood pressure in otherwise healthy people.
The study was published online Aug. 23 in the Journal of Neurology Neurosurgery & Psychiatry.
— Mary Elizabeth Dallas
Aug 17, 2017 | Healthy Tips
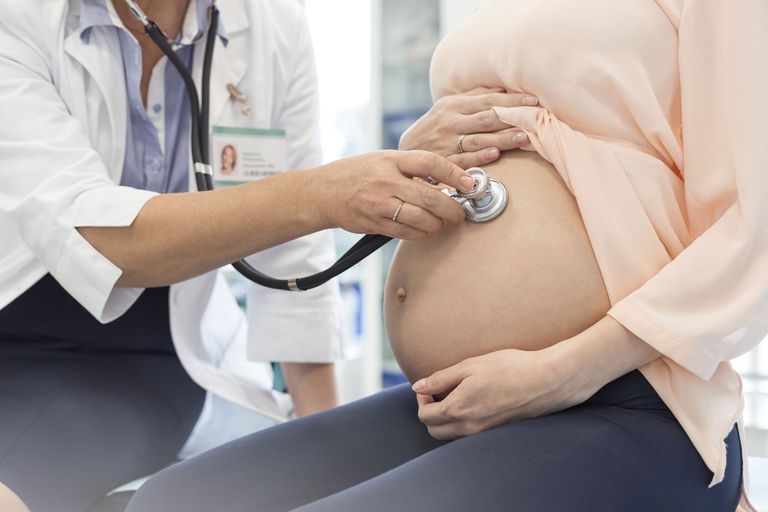
PREGNANCY COMPLICATIONS ASSOCIATED WITH PCOS
Risks To Mom And Baby And How You Might Prevent Them
By Nicole Galan, RN
Most women with PCOS are aware that they may have some difficulty becoming pregnant. Irregular periods and absent ovulation can make it challenging to time intercourse for pregnancy and commonly leads a couple to seek out the assistance of a reproductive specialist.
But many women aren’t aware that having PCOS can also increase her risk for certain pregnancy-related complications. Though rest assured these complications aren’t common, a woman should still visit her obstetrician regularly and follow her recommendations for prenatal screening.
Miscarriage
Women who have PCOS do appear to be at a slightly higher risk for having a miscarriage, though the cause for this relationship is unclear. Researchers believe that a few factors may be to blame. First, women with PCOS tend to have longer menstrual cycles, meaning that ovulation occurs later on. This exposes the developing egg to lots of hormones, possibly damaging it.
Second, there is a known relationship between uncontrolled blood sugar and miscarriage. Given that women with PCOS tend to have insulin resistance and elevated insulin levels, some researchers hypothesize that this may contribute to poor egg quality and miscarriage. High androgen levels and endometrial dysfunction, meaning problems with implantation, may also play a role in the increased risk of early pregnancy loss in women with PCOS – though more research is needed before a clear association can be developed.
Pregnancy-Induced Hypertension and Preeclampsia
Pregnancy-induced hypertension, or PIH, refers to women who develop new onset high blood pressure after 20 weeks.
Preeclampsia is a serious health condition that also develops in the second half of pregnancy and causes protein in the urine, in addition to high blood pressure. The loss of protein in the urine leads to swelling and signals a problem with the kidneys.
If left untreated, preeclampsia can progress to the severe form of the syndrome called eclampsia, which can cause seizures, blindness, and/or coma.
In serious cases, both maternal and foetal death can result.
Every time you visit your doctor, she will check your blood pressure and take a urine sample to look for protein in the urine. This is to make sure that you are not developing preeclampsia. If you are diagnosed with preeclampsia, treatment involves bed rest, frequent monitoring, and medication to hopefully lower your blood pressure. If your blood pressure does not decrease, the only known cure is to deliver the baby. The goal is to get the baby as far along in the pregnancy as possible so that the lungs have a chance to develop.
Women with PCOS tend to have higher blood pressure to begin with, increasing their risk for developing PIH. This is why it’s important to watch out for signs and symptoms of PIH and preeclampsia (swelling, rapid weight gain, severe headache, vision changes) and promptly report them to your doctor, or proceed to the emergency room if necessary.
Gestational Diabetes
Gestational diabetes occurs when diabetes, an alteration in how the body processes sugar, develops during pregnancy. While the condition usually resolves after giving birth, a woman with gestational diabetes is more likely to develop type 2 diabetes later in life, requiring ongoing monitoring of blood sugar levels.
All pregnant women are monitored for gestational diabetes with routine blood sugar screening sometime between 26 and 28 weeks. Women with known diabetes, insulin resistance, or who are at higher risk for developing gestational diabetes may be screened earlier. Women who are older than 25, have had gestational diabetes with prior pregnancies, who are overweight, who have prediabetes, or who have close family members who have been diagnosed with type 2 diabetes are at greater risk for developing gestational diabetes. Women with PCOS are a part of that group because of the association with insulin resistance and prediabetes.
Gestational diabetes can be treated with a combination of lifestyle changes or medication if necessary. It’s important to be vigilant about monitoring your blood sugar as directed by your physician because babies born to mothers with gestational diabetes are at higher risk for high birth weight, preterm birth, respiratory issues at birth, low blood sugar, and jaundice.
Premature Delivery
Women with PCOS are also at risk of delivering their baby early. The reason behind this again is not totally clear. Experts do know that preeclampsia is a risk factor for premature delivery, and women with PCOS are at a higher risk of preeclampsia.
In addition, experts have found that babies born to moms with PCOS are more likely to be large (called large for gestational age), have meconium aspiration (when a baby’s first stool gets into their lungs), and have a low Apgar score at five minutes.
Preventing Pregnancy Complications in PCOS
Some of these complications sound pretty scary, but there are many things that you can do to help prevent them. First and foremost is to get regular prenatal care as early into the pregnancy as possible. Even better would be to see your doctor before trying to conceive so that you can discuss specific steps to lower your risks – like optimizing your weight.
Second, make some positive lifestyle changes. Even though they may be hard to implement, remember that you are doing it for your baby (and for yourself). For instance, discuss an exercise regimen with your doctor, and if you struggle with healthy eating habits, ask for a referral to a nutritionist.
Sources:
American Diabetes Association. (2013). Before Pregnancy.
American Pregnancy Association. Polycystic ovarian syndrome.
Kamalanathan, S., Sahoo, J.P., & Sathyapalan, T. Pregnancy in Polycystic Ovary Syndrome. Indian Journal of Endocrinology and Metabolism, Jan-Feb;17(1):37-43.
Roos, N., Sahlin, K.H., Ekman-Ordeberg, G., Falconer, H., & Stephansson, O. (2011). Risk of Adverse Pregnancy Outcomes in Women with Polycystic Ovary Syndrome: Population-based Cohort Study. BMJ, Oct 13;343:d6309






