
Apr 1, 2026 | Healthy Tips

In the bustling markets and vibrant streets of Ibadan, a silent health crisis is unfolding, one that directly threatens the lives of our men. As an organisation based here in Oyo State, we are on the front line of the battle against non-communicable diseases (NCDs), particularly hypertension and diabetes. Every day, we witness a disturbing trend: today, men—especially young adults with bright futures, careers, and families—are dying daily from preventable health issues directly linked to the consumption of trans fats.
This is not just a health issue; it is a crisis that is robbing our community of its fathers, brothers, and leaders.
Trans fats, or trans-fatty acids, are the most dangerous type of fat for the human heart and vascular system. They are primarily created in an industrial process that adds hydrogen to liquid vegetable oils to make them more solid. For food vendors and producers, this is a cheap and attractive option because it increases the shelf life and flavour stability of foods.
In Ibadan, common sources of industrially produced trans fats include:
Reused Frying Oils! Oils are used repeatedly to fry popular staples like akara (bean cakes), puff-puff, boli (roasted plantain) with groundnut oil, and doughnuts sold by roadside vendors.
Margarines and Vegetable Shortenings! Often used in baked goods like bread, cakes, and pastries sold in local bakeries.
Packaged Snacks? Some commercially fried snacks and fast foods.
Our work at the Rays of Hope Support Initiative has highlighted a critical and concerning pattern: the devastating impact of trans fats is not gender-neutral.
While women are not completely immune, their natural hormonal makeup, particularly oestrogen, offers a degree of protection by helping to regulate cholesterol levels and fat distribution. This biological advantage, however, is not shared by men.
The male body is particularly vulnerable. In our screenings across Ibadan, we have observed that the majority of our men tend to develop visceral fat—the dangerous fat that accumulates deep within the abdomen, wrapping around their internal organs. This is the direct consequence of a diet high in trans fats. This central obesity is a ticking time bomb, leading to a cascade of life-threatening complications:
Trans fats wreak havoc on a man’s lipid profile. They raise “bad” cholesterol (LDL) and lower “good” cholesterol (HDL). They also significantly increase triglycerides, another type of fat in the blood that hardens arteries.
Also, the build-up of cholesterol and triglycerides doesn’t just sit idly on our body. It forms plaque, leading to the narrowing and hardening of our arteries (atherosclerosis)—”a sure path to hypertension”. The heart is then forced to pump blood through these constricted pathways, leading to dangerously high blood pressure (hypertension)—a condition we see daily at our centre.
Visceral fat is not inert; it acts like an active organ, releasing inflammatory substances that make the body’s cells resistant to insulin. This insulin resistance is a direct precursor to high blood sugar and type 2 diabetes, creating a perfect storm where a man is now managing two or more debilitating NCDs simultaneously.
The result is a preventable tragedy—a young man in his 30s or 40s, a provider for his family, suffers a sudden heart attack or stroke or is diagnosed with advanced kidney disease from uncontrolled hypertension and diabetes. Hmmm!
Addressing this crisis requires a multi-pronged approach, from individual lifestyle changes to systemic action by authorities.

Here is what needs to be done:
For Individuals and Families:
Dietary Overhaul:
- Minimise the consumption of foods fried in oil that has been used repeatedly. Be mindful of the deep golden-brown colour of repeatedly heated oil used for frying akara and puff-puff.
- When buying packaged foods, look for “partially hydrogenated oils” on the ingredient list—this is a direct indicator of trans fats.
- At home, use healthier oils like olive, soybean, or palm oil in moderation, and avoid heating them to the smoking point.
- Aim for at least 150 minutes of moderate-intensity exercise per week. This could be a brisk walk around your neighbourhood, cycling, or engaging in local group sports. Exercise is the most effective way to burn visceral fat.
- Do not wait for symptoms. As an organisation working within the NCDs healthcare space, we cannot overemphasise the importance of regular check-ups. Know your numbers: blood pressure, blood sugar, and cholesterol levels. Early detection is the only way to intervene before complications arise.
- If diagnosed with hypertension or diabetes, it’s not a death sentence but a lifelong condition that requires consistent management. Take your medication exactly as prescribed by a healthcare professional. Do not stop when you feel better; consult your doctor and dietitian first.
To our government (Oyo State and Federal):
Nigeria must implement and enforce a trans fat ban by leading other nations in setting a legal limit for industrially produced trans fat in all foods.
Enforce strict quality controls on the production and sale of cooking oils to prevent adulteration and promote healthier options.
Launch mass media campaigns (radio, TV, town criers) in local languages to educate the public, especially men, about the dangers of trans fats, using culturally relevant examples like akara and puff-puff.
To our healthcare centres and authorities:
Every consultation for hypertension or diabetes must include practical, actionable advice on avoiding trans fats. We are asking for integrated dietary counselling.
Equip community health workers and nurses with the knowledge to counsel patients on healthy cooking practices and food choices.
Improve the tracking and reporting of NCDs to the appropriate quarters so as to better understand the scope of the problem.
To organisations working within the health care space:
We must continue to take our services to the markets, motor parks, and communities, meeting men where they are to check their blood pressure and blood sugar.
Develop programmes specifically for men, focusing on the link between their diet (e.g., the oil in their favourite local foods) and their future health. Use relatable language and peer-to-peer influence.
We must collectively raise our voices to urge the government for stricter regulations on trans fats. We are the voice for the communities we serve.
Create and facilitate support groups for men living with hypertension and diabetes, providing a space for shared learning and encouragement.
The fight against trans fats is a fight for the future of our men in Ibadan and Nigeria. Through awareness, lifestyle change, and strong advocacy, we can reverse this trend and ensure that our young men live to fulfil their promising futures.

Apr 1, 2026 | Healthy Tips

Hello, ROHSI Community! When we talk about diabetes, it’s important to know what can happen if our blood sugar is not well managed. Having too much sugar in our blood for a long time can slowly damage our blood vessels and nerves. This can lead to other health problems.
But please, don’t be afraid! These problems are not something that will definitely happen to you. There is a lot we can do to prevent them. By taking our medication as prescribed and building good daily habits, we can keep our diabetes under control and stay healthy.
What Happens When Diabetes Is Not Controlled?
Think of high blood sugar as something that can quietly affect many parts of our body. Here’s what we need to watch out for:
- Our Eyes! High blood sugar can make it harder to see and can even lead to blindness. It can cause problems like:
- Cataracts! Cataract surgery is when the lens of our eye becomes cloudy, like looking through a dirty window.
- Glaucoma! This damages the nerve that connects our eye to our brain.
- Retinopathy! This is damage to the back part of our eye (the retina).
- Our Heart! Over time, high blood sugar can harm the blood vessels and nerves that control our heart. This makes us more likely to have heart disease, a heart attack, or a stroke. If we also have high blood pressure or high cholesterol, the risk is even higher.
- Our kidneys! Our kidneys are like filters for our body. Diabetes can damage the tiny blood vessels in these filters, making them work less effectively. After many years, if the damage is severe, the kidneys can stop working altogether.
- Our Feet! High blood sugar can slow down blood flow and cause nerve damage in our feet. This is very dangerous because:
- You might not feel pain from a cut, blister, or sore.
- Because of poor blood flow, these small injuries can heal very slowly and become infected easily.
- If a bad infection cannot be treated, it might lead to a doctor having to remove a toe, a foot, or part of the leg.
- Our Nerves! When high blood sugar damages our nerves (this is called diabetic neuropathy), it can cause pain, tingling, or numbness. This is most common in the hands and feet.
- Our Skin! Diabetes can make us more likely to have dry, itchy skin, yeast infections, or dark, scaly patches on the skin.
- Erection Problems for Men! High blood sugar damages the blood flow and nerves needed for a man to get and keep an erection. This is a common problem for men with diabetes.
What Can We Do to Stay Safe?
The good news is that we have a lot of power to protect ourselves. By making these simple steps a part of our daily life, we can greatly lower our risk of these problems.
Control Your Blood Sugar! This is the most important thing you can do. Aim to keep your numbers within a healthy range. Check your sugar as your doctor advises and try to keep it
- Between 70 and 130 mg/dL before meals.
- Less than 180 mg/dL two hours after a meal.
- Your A1C (which shows your average blood sugar over 3 months) should be below 7%.
Watch Your Blood Pressure and Cholesterol! High blood pressure and cholesterol are a dangerous mix with diabetes. Work with your doctor to keep them under control, which might include taking medication. A good target is to keep your blood pressure below 140/90 and your total cholesterol at or below 200.
See Your Doctor Regularly! Don’t wait until you feel sick. Regular checkups are vital because many diabetes problems start without any warning signs. Your doctor can test your blood, urine, and eyes to catch any issues early.
Don’t smoke! Smoking is very bad for your blood flow and raises your blood pressure, making diabetes complications much worse. If you smoke, ask your doctor for help to quit. It’s the best thing you can do for your health.
Protect Your Eyes! Get your eyes checked by a professional at least once a year. They can look for early signs of damage and start treatment right away.
Check Your Feet Every Day! Make this a habit!
- Look for any cuts, sores, blisters, redness, or swelling, especially between your toes and on the bottom of your feet.
- Wash your feet daily with warm (not hot) water and dry them carefully, especially between the toes.
- Apply lotion to keep the skin soft and prevent cracks, but not between the toes.
- Always wear shoes to protect your feet, even at home. Never walk barefoot on hot ground or at the beach.
- Trim your toenails straight across and file the edges gently.
- Always test bathwater with your hand or elbow first to avoid burning your feet.
Take Care of Your Skin:
- Keep your skin clean and dry, especially in areas like your armpits.
- Use talcum powder to prevent rubbing and chafing.
- Avoid very hot baths and strong, drying soaps.
- Use body lotion to keep your skin from getting too dry and cracking.
Let’s take these steps together, for ourselves and for our community. We can live well with diabetes! Also, we need to remember that many diabetes problems don’t shout; they creep in quietly. This is why regular checkups at the clinic are your best defence!
Courtesy: WebMD and Rays of Hope Support Initiative (ROHSI)

Mar 3, 2026 | Healthy Tips

Do we know that familiarising ourselves with the following basic health principles in 2026 will most likely help you and me stay out of the hospital or pharmacy or even avoid taking medication due to illness? Yeah
* Very cold water at dawn shocks the stomach like bad news. Let’s start our morning gently with a glass of warm or room-temperature water.

* Our cooking oil should assist our food, not announce itself before the meal arrives. In 2026, we must use oil moderately, like what my dietitian used to say: ‘If it dropped on your clothes or water paper, it would show.’ That is how our cooking oil should be when using it to make soup. Remember to ask or talk to your dietitian about the best cooking oil to go for.
* We must be ready to negotiate our daily rice intake with alternative food items. Eating rice daily is like gradually inviting diabetes, so we must be ready to vary our diet.
* Eating heavy meals at midnight is telling our heart to work overtime without pay, and sleeping immediately after eating is like parking a moving car. In 2026, we must try to stop late-night eating. Let’s maintain at least 3 hours between mealtime and bedtime.
* Speed eating is a modern sport with no trophy. You and I must learn to chew our food like we paid for it. Swallowing our food in a hurry is disrespectful to digestion. We must take our time when eating. Our mouth is not a shortcut; it is our first doctor. Digestion starts on our tongue.
* If our legs still work, we must be ready to use them properly in 2026. Every unnecessary short ride is a missed blessing. When the trip is super short, let’s park the car and walk around the block. It doesn’t mean you are poor or can’t show off with pride, but look at the health aspects associated with such an action of yours.
* Stretching in the morning tells our joints, “We have not abandoned you.” If we won’t do extensive exercise every day, at least let’s learn to stretch our joints daily.
* Sweeping our house and doing basic house chores is not punishment. It is unpaid physiotherapy. Sweeping, cleaning, and washing are exercises disguised as responsibilities. We don’t have to outsource everything. Do some ourselves to move our joints and muscles.
* This year, we must make it a must to sit with our healthcare providers. We must see medical checkups as routine when they’re recommended and not mean we are weak. It means we are intelligent and conscious. A small sickness we ignore today becomes a big hospital bill tomorrow. So, it’s a must for us to at least sit with our healthcare providers in respect to our annual medical checkup.
* Water is life, yes. Thirst is a late warning. We must learn to drink water regularly before thirst arrives. We must always move with water. Sip water at an interval if possible. This year we must drink water like maintenance, not like rescue.
* Rest is not laziness. It is wisdom to wear comfortable clothes. Sleep well every night. No lights and no radio or TV on. Light at night confuses the brain. Even our phone needs dark mode. Just total darkness and our pillow.
* If our food cannot trace its ancestry to a village, a farmer, or a season, our body will struggle to recognise it. Garden eggs and okra may not trend on social media platforms, but our blood pressure respects them deeply. Eat more fresh foods and fewer processed foods. Yeah
* Life is already sweet enough. Bitter leaf, neem, sour soup, scent leaves, and prekese remind the liver that discipline still exists. Once in a while, take these in moderation.
* Before today’s modern transportation system, legs were the original transport system. Walking is not poverty; it is preventive medicine. If we avoid walking, we are avoiding good health. So, go get your jogging kits ready without an excuse.
* Anger does not punish the offender; it poisons the host quietly. Be mindful of our emotions and mental health in 2026.
* We must not turn insecticide into perfume. Excess chemicals do not kill only mosquitoes; they confuse our lungs too. We must use them in moderation and do nets.
* If our stomach refuses to talk daily, something is wrong. Constipation is the body holding grudges. Let’s check our eating habits and lifestyle and resolve the strike immediately before it turns bloody.
* We must learn to manage stress intentionally. Stress is useful only in emergencies, not as a daily occurrence. Fatigue is not discipline. Learn to take short breaks during work.
* Avoid constant snacking. The stomach also needs rest. Digestion is work. Too much work causes fatigue.
ROHSI Management Team.

Feb 15, 2026 | Healthy Tips

How diabetes and cancer are linked, why cancer survivors face diabetes risk, and what new-onset diabetes may reveal about hidden cancers.
By Justine Evans
Some facts about diabetes and cancer:
- Type 2 diabetes increases risk for certain cancers.
- Some cancer treatments may cause diabetes later.
- New-onset diabetes in older adults may signal hidden cancer.
- Screening and lifestyle changes can reduce risk.
- Research is exploring new diagnostic tools using these links.
If you’re living with diabetes, you might know all about the intriguing and intricate relationship between diabetes and certain types of cancer. And it’s not a one-way street — the connection goes both ways.
So, what does current research say about this bidirectional relationship? Why are some cancer survivors more likely to develop diabetes? And why is understanding the difference between new-onset and long-standing diabetes critical in cancer detection and care?
Which cancers are linked to diabetes?
It’s been known for some time that diabetes, especially type 2 diabetes, can increase the risk of several types of cancer. But which cancers specifically?
According to a growing body of evidence, people with diabetes are more likely to develop pancreatic, liver, colorectal, breast and endometrial cancers. Why these cancers in particular? Different factors may be at play:
- People with type 2 diabetes often have higher circulating insulin levels, which may promote the growth of cancer cells.
- Long-term low-grade inflammation, common in diabetes, can create an environment in the body that’s more vulnerable to cancer development.
- Persistently high glucose levels may not only damage blood vessels and organs but also contribute to tumour growth.
A 2025 review in Seminars in Oncology outlines these mechanisms in detail, underscoring that this isn’t just correlation butthe risk that there’s a plausible biological basis linking diabetes to cancer risk.
It’s been known for some time that diabetes, especially type 2 diabetes, can increase the risk of several types of cancer. But which cancers specifically?
The gender gap in diabetes-related cancer risk
Diabetes doesn’t affect everyone’s cancer risk in the same way. In fact, research shows that women with diabetes tend to have a higher overall risk of developing cancer than men with diabetes. Across many different cancer types, the relative increase in cancer risk associated with diabetes was greater in women. Importantly, this wasn’t limited to a single cancer. Instead, diabetes appeared to place a broader cancer burden on women overall.
So why might this difference exist? The answer is likely complex and involves a mix of biological and lifestyle factors. Many of the risk factors shared by diabetes and cancer, such as excess body weight, physical inactivity and smoking, can worsen insulin resistance and promote long-term inflammation in the body.
These changes can also disrupt hormone regulation, all of which are processes linked to cancer development. Some evidence suggests that these metabolic and lifestyle effects may be more pronounced, or persist for longer, in women with diabetes. Over time, this may help explain why women experience a greater relative increase in cancer risk compared with men, even when both are living with the same condition.
Can cancer treatments cause diabetes?
Interestingly, the relationship works the other way, too. People who have survived cancer, particularly those treated with certain therapies, are at greater risk of developing new-onset diabetes after cancer.
A recent article published in Annals of Medicine and Surgery (2024) explored how cancer treatments, while life-saving, can disrupt glucose metabolism in various ways. Here are a few examples:
- Chemotherapy and corticosteroids, often used to manage cancer or treatment side effects, can cause spikes in blood sugar.
• Androgen deprivation therapy (used in prostate cancer) has been associated with insulin resistance.
• Abdominal radiation, particularly in children and young adults, can damage the pancreas, impairing insulin production.
This risk is beyond a simple short-term issue during treatment. For many survivors, diabetes may not appear until months or even years later. And because cancer follow-up typically focuses on recurrence and surveillance imaging, blood glucose levels might not be closely monitored unless there’s a specific concern.
People who have survived cancer, particularly those treated with certain therapies, are at greater risk of developing new-onset diabetes after cancer
It’s not just a case of better detection
You might ask whether there is simply an increase in diabetes and cancer diagnoses because we’re looking more closely. After all, both conditions are common, and frequent medical visits often lead to more testing. But experts now agree this is more than just detection bias. A growing number of studies demonstrate a biologically plausible connection between the two conditions.
For instance, shared risk factors, such as obesity, sedentary lifestyle, poor diet, and inflammation, as well as treatment-related effects that support this real, bidirectional link. Although these shared risk factors present a more complex picture, the association between diabetes and certain cancers remains.
That means clinicians are not just diagnosing more people by chance. There is a real link that has clinical implications for diabetes management and cancer care.
New-onset vs long-standing diabetes: a new focus in research
Here’s where it gets even more interesting. Researchers are now focused on distinguishing new-onset diabetes, especially in older adults, as a potential early marker of underlying cancer, particularly pancreatic cancer.
Why pancreatic cancer? Because in many cases, new-onset diabetes can precede the cancer diagnosis. The pancreas is central to both insulin production and tumour development, and a pancreatic tumour can impair insulin secretion, sometimes months before the cancer is detected.
So, while long-standing diabetes may increase the risk of developing certain cancers over time, sudden-onset diabetes, especially in someone with no history of obesity or insulin resistance, could be a red flag. This is especially important because pancreatic cancer often presents late and has poor survival outcomes. Early detection can make a big difference.
In fact, healthcare systems are exploring screening programmes that use new-onset diabetes in people over 50 as a trigger to investigate for pancreatic cancer. It’s a promising area of research that could lead to earlier diagnoses and better outcomes.
Sudden-onset diabetes, especially in someone with no history of obesity or insulin resistance, could be a red flag
What does this mean for people living with diabetes or cancer?
Understanding this bidirectional relationship matters for individuals and healthcare providers.
- If you have diabetes: Regular cancer screenings, especially for colorectal, breast, and liver cancers, may be more relevant than ever. Maintaining good glycaemic control, staying active and managing weight could help reduce your risk.
- If you’re a cancer survivor: Keep an eye on your blood glucose levels, even years after treatment. If you were exposed to chemotherapy, steroids, radiation, or hormone therapy, you may have a higher chance of developing diabetes, and early diagnosis is key.
- If you’re newly diagnosed with diabetes in your 50s or older: Talk to your GP about whether further investigation might be needed, particularly if you don’t fit the type 2 diabetes profile. It might be nothing, but it’s worth checking.
What’s next in research?
The complex interaction between diabetes and cancer is now one of the most dynamic areas of medical research. With a better understanding, there’s hope that:
- Cancer therapies are refined to reduce metabolic side effects.
- New-onset diabetes can serve as a valuable biomarker for early cancer detection.
- Strategies are developed to prevent diabetes in cancer survivors through tailored screening and lifestyle support.
It’s a reminder that in medicine, everything is connected, and sometimes the clues to one condition or disease lie in the symptoms or progression of another.
In medicine, everything is connected, and sometimes the clues to one condition or disease lie in the symptoms or progression of another.
Should people with diabetes be alarmed?
Living with diabetes doesn’t mean you’re destined to develop cancer, and not all cancer survivors will go on to develop diabetes. But recognising the links between these conditions can empower you to take preventive action, ask informed questions, and work with your healthcare team for more personalised care.
After all, the more we understand how diseases interact, the better we can treat and prevent them.
https://diabetesvoice.org/en/caring-for-diabetes/diabetes-and-cancer-whats-the-real-connection/?mc_cid=0daf1860af&mc_eid=50b74717d8

Feb 14, 2026 | Healthy Tips
Anita Sabidi

The myth of the supermom: embracing vulnerability with Type 1 Diabetes
Motherhood is often painted as a story of strength, resilience, and endless sacrifice. As mothers, we are expected to be the pillars of our families—the ones who hold everything together no matter what. But living with Type 1 diabetes for more than two decades has taught me that being a mother does not mean being invincible. In fact, one of the most valuable lessons I’ve been able to share with my children is that their mama is not a superwoman. I can be strong, yes, but I can also be vulnerable. And that’s okay.
Type 1 Diabetes is a family affair: when daily rituals become childhood memories
Every day with diabetes is a balancing act. Managing insulin, blood sugar checks, and the unpredictability of the condition can feel like carrying an invisible load. Yet this journey is not mine alone—it has become a family affair. My children have grown up witnessing my daily rituals with insulin injections and blood glucose monitoring. What might seem routine to me is part of their childhood memories, shaping how they understand care, responsibility, and empathy.
“Cover mama!”: how my kids became my little bodyguards
One of the sweetest moments happens whenever it’s time for my insulin shot in public. Without being asked, my kids instinctively take position around me, shielding me from curious stares. “Cover Mama!” they say, forming a protective circle as I inject. In those little moments, I see their love, their awareness, and their willingness to step into the role of supporters. They are my little bodyguards, and I treasure that more than words can describe.
Why sharing my needs is a lesson in strength, not a burden
Some might think children shouldn’t have to carry that kind of responsibility. But I see it differently. By sharing my vulnerabilities with them, I am teaching them important lessons about life: that strength is not about pretending to be unbreakable, but about acknowledging our needs and asking for support. That caring for one another is not a burden, but an act of love.
Authenticity over perfection: what my children taught me about Type 1 Diabetes resilience
Motherhood with diabetes has also shown me that I don’t have to live up to the impossible standard of being a superwoman. My kids don’t need perfection; they need authenticity. They need to see that it’s human to struggle, to adapt, and to keep going despite the challenges. They need to know that resilience comes not from denying vulnerability, but from embracing it.
So yes, I am a mother living with diabetes. I am a caregiver, but I am also someone who needs care. And in this shared journey, my children and I are learning together—that family is not about one person carrying it all, but about supporting each other through life’s highs and lows.
Conclusion
In the end, I hope my children grow up knowing this truth: that their mama’s greatest strength is not being superhuman but being real.
https://hellotype1.com/en/articles/motherhood-and-type-1-diabetes-why-showing-vulnerability-made-me-a-stronger-mom
Sep 1, 2025 | Healthy Tips

Cholangiocarcinoma, also known as bile duct cancer, is a rare and aggressive form of cancer that originates in the bile ducts. These ducts play a crucial role in digestion by transporting bile from the liver to the gallbladder and small intestine. Bile is a fluid that helps the body digest fats.
Benjamin Olorunfemi
Cholangiocarcinoma, also known as bile duct cancer, is a rare and aggressive form of cancer that originates in the bile ducts. These ducts play a crucial role in digestion by transporting bile from the liver to the gallbladder and small intestine. Bile is a fluid that helps the body digest fats.
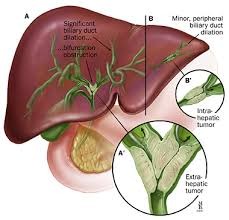
Cholangiocarcinoma cancer is classified based on its location:
- Intrahepatic cholangiocarcinoma! Begins in the bile ducts within the liver.
- Extrahepatic cholangiocarcinoma! Begins in the bile ducts outside the liver and is further divided into perihilar (at the point where the main bile ducts leave the liver) and distal (further down the bile duct).
A key challenge with this cancer is that it often doesn’t show symptoms in its early stages. By the time symptoms appear, the cancer has often spread, making it difficult to treat effectively.
Currently, there’s no strong evidence showing a major surge in cholangiocarcinoma specifically in Nigeria or among people of African descent. However, some risk factors linked to this cancer (like liver fluke infections, hepatitis B/C, and cirrhosis) are present in Nigeria, which could contribute to cases.
Symptoms of cholangiocarcinoma can be subtle and often don’t appear until the disease is advanced. They can include:
- Jaundice (yellowing of the skin and whites of the eyes)
- Itchy skin
- Dark urine and pale, greasy stools
- Unexplained weight loss and loss of appetite
- Abdominal pain, especially on the right side under the ribs
Treatment options depend on the stage and location. They can include:
- Surgery! The primary treatment, when possible, is to remove the tumour. This may involve removing a portion of the bile duct or even part of the liver.
- Liver Transplant! In some specific cases, a liver transplant may be a curative option, particularly for certain types of hilar cholangiocarcinoma.
- Chemotherapy! Uses drugs to kill cancer cells and can be used to slow the disease and relieve symptoms in advanced cases.
- Radiation Therapy! Uses high-powered energy beams to destroy cancer cells.
- Other therapies! These can include targeted drug therapy, immunotherapy, or procedures like biliary drainage to relieve symptoms caused by blockages.
Challenges in Nigeria
Survival rates for cholangiocarcinoma in Nigeria are low due to several challenges, including:
– Late diagnosis! Many cases are diagnosed at an advanced stage, making treatment more difficult.
– Limited access to healthcare! Many Nigerians lack access to quality healthcare services, including cancer diagnosis and treatment.
– Lack of awareness! There is a need for increased awareness about cholangiocarcinoma and its symptoms.
– Alcohol & Aflatoxin Exposure! Heavy alcohol use and contaminated foods (like poorly stored grains) increase liver disease risk.
– Financial Barriers! The cost of diagnostics and treatment is often a major hurdle for patients. Without adequate health insurance or government support, many people simply cannot afford the care they need.
– Weak Advocacy! While cancer advocacy groups are growing in Nigeria, the movement is still in its early stages. Stronger advocacy is needed to prioritise cancer control on the national health agenda.
Ways Out (Solutions):
- Better Awareness – Educate people on symptoms (jaundice, abdominal pain, weight loss).
- Early Screening – Regular check-ups for high-risk groups (hepatitis patients, those with liver disease).
- Improved Sanitation – Reduce liver fluke infections with clean water and food safety.
- Vaccination – The hepatitis B vaccine can lower liver cancer risks.
- Access to Treatment – More cancer centres and affordable care for early detection and surgery/chemotherapy.
- Support research: Encourage research into the causes and treatment of cholangiocarcinoma.
Cholangiocarcinoma is rare but deadly, especially when caught late. Early detection saves lives. So, if someone has prolonged jaundice, unexplained weight loss, or severe itching, they should see a doctor immediately.
The ROHSI team is saying you can help in this fight against the surge of cancer-related help by:
- Share this article and other resources about cholangiocarcinoma with your network.
– Offer emotional support and connect individuals with resources and services.
– Advocate for increased funding and resources for cholangiocarcinoma research and treatment.
Together, we can make a difference and improve the lives of those affected by cholangiocarcinoma in Nigeria. Get involved today.
Rays of Hope Support Initiative (ROHSI)









